Each of our hospital-based rehabilitation clinics is staffed by highly-experienced and credentialed therapists using the most advanced tools and modalities. Our therapists are dedicated to helping you achieve your highest level of recovery and independence. All of our therapies require a doctor’s referral and are available in an inpatient and outpatient setting. Please note, however, that each hospital offers varying treatment modalities, so your doctor may recommend one over another based on your particular rehabilitation need.

Bon Secours St. Francis Hospital
- Physical therapy
- Occupational therapy
- Speech therapy
- Aquatic therapy
- Lymphedema therapy (provided by certified therapist)
- Dry needling
- Modalities
- Stroke rehab
- Hand therapy/splinting
- Cervical and lumbar traction
- Gait and balance training
- Manual therapy
- Kinesiotaping
- Strengthening and conditioning for specific areas of weakness
For more information on services offered at Bon Secours St. Francis Hospital call (843) 402-2014
Roper Hospital
- Physical Therapy
- Occupational Therapy
- Speech Therapy
- Brain Injury Specialty Program accredited by the Commission on Accreditation of Rehabilitation Facilities
- Spinal Cord Injury Specialty Program accredited by the Commission on Accreditation of Rehabilitation Facilities
- Center for Spinal Cord Injury
- Wheelchair clinic (physicians order needed)
- Driving program and evaluation
- Lymphedema therapy (provided by a certified therapist)
- Activities of daily living training
- Hand therapy
- Splinting
- Gait and balance training
- Dry needling
- Kinesiotaping
- Cervical and lumbar traction
- Modalities including electrical stimulation, ultrasound and iontophoresis
- Neuromuscular therapy
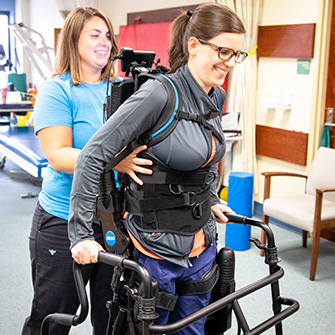
- Exoskeleton (provided by a certified therapist) – Exoskeleton device allows therapist to gait train patients working toward household and community ambulation goals. It allows therapists to focus on quality and minimize deviations while a patient actively relearns a quality gait pattern.
- Graston Technique therapy can be used on soft tissue injuries whether they are chronic, acute or post-surgical. The unique instruments help with scar tissue and fascial restrictions that help with motion, decreasing pain and restoring function.
- Bioness (provided by a certified therapist)
- FES cycle (provided by a certified therapist)

For more information on services offered at Roper Hospital call (843) 724-2870
Roper St. Francis Berkeley Hospital
- Physical therapy
- Occupational therapy
- Speech therapy
- Cervical and lumbar traction
- Modalities including electrical stimulation, ultrasound and iontophoresis
- Neuromuscular therapy
- Activities of daily living training
- Hand therapy
- Splinting
- Gait and balance training
For more information on services offered at Roper St. Francis Berkeley Hospital call (854) 529-3190
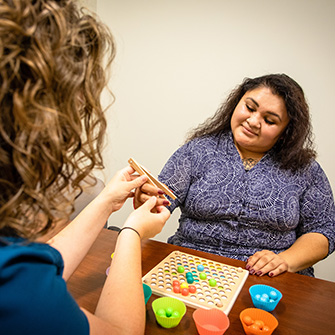
Roper St. Francis Mount Pleasant Hospital
- Physical therapy
- Occupational therapy
- Dry needling
- Modalities
- Stroke rehab
- Cervical and lumbar traction
- Gait and balance training
- Manual therapy
- Kinesiotaping
- Strengthening and conditioning for specific areas of weakness
For more information on services offered at Roper St. Francis Mount Pleasant Hospital call (843) 606-7605